|
Orthologix brings you quarterly information to keep you current on industry news, trends and insights. Orthologix is an orthotics and prosthetics practice delivering evidence-based care throughout the Delaware Valley.

Pediatric Upper Limb Prostheses - Myoelectrics
 The CDC estimates that each year about 1,500 babies in the United States are born with upper limb reductions or congenital amputations– 4 out of every 10,000.
With effective orthopedic and ancillary support, most children with an incomplete upper limb can lead normal lives. The CDC estimates that each year about 1,500 babies in the United States are born with upper limb reductions or congenital amputations– 4 out of every 10,000.
With effective orthopedic and ancillary support, most children with an incomplete upper limb can lead normal lives.
Although a child’s prosthesis has the same components as an adult’s, pediatric patients require special design considerations to not only have the prosthesis fit comfortable and securely, but to be fit and fabricated for a child’s natural growth and development.
During the past quarter century, many changes and modifications in children’s prostheses have occurred to contribute to the highest possible standard of quality of life, allowing children to participate in nearly all the same activities, sports, and recreation as their contemporaries.
However, an upper-limb prosthesis for children comes with unique challenges and considerations.
Gerald Stark, MSEM, CPO/L, FAAOP, Senior Upper Limb Clinical Specialist for Ottobock, explains in his comments below the process of fitting the child with a prosthesis and the role occupational therapists play in a child having a successful outcome.
‘Sit to Fit’
The age when a child should begin wearing a prosthesis greatly differs among clinicians. The prevailing opinion until 8-10 years ago was to fit when the child was sitting-up. The expression many clinicians used was ‘Sit to Fit.’ This meant that the child was fit with their first passive device as early as 3-6 months because they were ready for bimanual tasks and to explore the world around them. This first passive device may be a simple rubber type hand and wrist to help with crawling and protection as the child begins to ambulate. The arm was then activated at roughly 1.5 years for a below-elbow limb deficiency and 3 years for an above-elbow limb deficiency.
The major issue is componentry: the hand, wrist, and elbow needs to be small enough to use for the patient and that it accommodates them as they grow.
This decision to fit early on in childhood has been recently criticized by some who say the fitting should only occur when the child inquires about it for functional reasons; however, others indicate that early intervention lets the child incorporate the device into their body image and sense of symmetry at an earlier age.
Consideration of length of limb
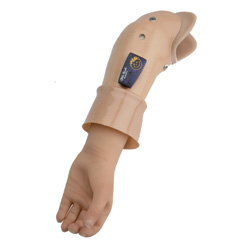 Length is definitely a consideration for any prosthesis including children. For the most part approximately 70% of all limb deficiencies for children are female, left, and below-elbow. This is considered “idiopathic” in that we really don’t know why this is. It has been suspected that it is due to hormonal levels during in vitro growth for girls and mothers that may cause lack of limb bud development. The typical length is short to very short for this level. However, there are definitely other levels of amputation that have small vestigial finger remnants or “nubbins” that can be used to control the prosthesis. Length is definitely a consideration for any prosthesis including children. For the most part approximately 70% of all limb deficiencies for children are female, left, and below-elbow. This is considered “idiopathic” in that we really don’t know why this is. It has been suspected that it is due to hormonal levels during in vitro growth for girls and mothers that may cause lack of limb bud development. The typical length is short to very short for this level. However, there are definitely other levels of amputation that have small vestigial finger remnants or “nubbins” that can be used to control the prosthesis.
The prosthetist must make certain accommodations for this limb length with respect to the battery, control electronics, wrist and hand mechanisms, as well as the construction of the arm. There is usually space between the interface and the components at the end of the prosthesis, but often this is limited with children who have proportionately small limbs to an adult. For example, a child may only be able to touch their fingers over their head, which indicates how much smaller their arms are compared to adults.
Benefits of wearing a prosthesis at an early age
The benefits of introducing a prosthesis at an early age have been listed by earlier studies.
These include the development of bimanual tasks and motor skills as the child begins to explore the world around them rather than just using a single arm. Another is for the development of ambulation so they have an arm that can be extended to aid in crawling and walking as they pull to stand and “cruise” from one object to another. Along with this is protection as they inherently experience falls so they have an arm out in front of them so they can catch themselves.
Also the child begins to incorporate the prosthesis into their sense of body imagery and symmetry. The child develops a sense of “projected kinesthesia” in that the prosthetic arm becomes more part of their cognitive development and brain motor development. The ultimate hope is that the child is able to use the arm routinely for more complex bimanual tasks that require a high degree of dexterity such as drawing, arts, dressing, or tying shoes.
Occupational Therapy
Early intervention by an experienced Occupational Therapist is indicated to help develop these skills. The prosthetist and OT work together as a clinical team to address various needs as they develop. The OT should be visited on a weekly then monthly basis as first to keep up with the child’s adjustment to the prosthesis.
The parents play a critical role to record any issues with the prosthesis that may cause frustration by the patient. The OT will attempt to recreate the same situations and attempt to resolve them with new gripping and activity strategies. The pediatric prosthetic user can then practice these activities to develop new skills and proficiencies.
Prosthetic improvements and advances
 There have been numerous improvements to componentry and fabrication of prostheses that make them more comfortable for the active lifestyle of children. The first is the interface design that has become softer and more flexible due to improvements with hybrid thermoplastics and silicone rubbers. This allows for a much more intimate fit that can flex with the child’s movements. As an added benefit these are often much easier for the child to put on and take off. There have been numerous improvements to componentry and fabrication of prostheses that make them more comfortable for the active lifestyle of children. The first is the interface design that has become softer and more flexible due to improvements with hybrid thermoplastics and silicone rubbers. This allows for a much more intimate fit that can flex with the child’s movements. As an added benefit these are often much easier for the child to put on and take off.
Another benefit are composite materials that make the prosthesis very light weight and durable. Durability is extremely important for children because they are just as active as Paralympic athletes in the types of activities they do. The prosthesis should be able to tolerate handstands, play gym climbing, soccer, baseball and any other activity the child wishes to experience.
A strong, durable, and yet cosmetic glove covering is also important. New advances in urethane and silicone as well as protective coatings, allow for greater flexibility with durable performance. Although the glove will need to be replaced periodically due to wear and staining, the life of the glove can be extended with new materials.
Gloves come in 18 different colors to match the skin shade of the child. Recently new glove colors of blue, yellow, red, and pink have been introduced since kids think “outside of the box” and wanted hands with different colors. Also new designs in batteries and motors allow the same durability with greater grip strength and speed than previous designs. More intricate machining and design practices make it possible to deliver more durable and lighter weight componentry as well.
Back to top

CASE STUDIES
Egermann M, Kasten P, Thomsen M (2008) Myoelectric hand prostheses in very young children. Int Orthop. 2009 Aug; 33(4): 1101–1105.
Abstract: Myoelectric prostheses have generally been provided for adolescent or adult patients.
The availability of smaller-sized electric hands has enabled the introduction of myoelectric prostheses to preschool children, mainly in the Scandinavian countries. This study evaluates the acceptance of myoelectric prostheses in 41 children with unilateral upper limb deficiency between the ages of two and five years. The prosthesis was used for an average time of 5.8 hours per day. The level of amputation was found to influence the acceptance rate. Furthermore, prosthetic use training by an Occupational Therapist is related to successful use of the prosthesis. The general drop-out rate in preschool children is very low compared to adults. Therefore, infants can profit from myoelectric hand prostheses. Since a correct indication and an intense training program significantly influence the acceptance rate, introduction of myoelectric prostheses to preschool children should take place at specialised centres with an interdisciplinary team. To read more: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2898999/
Shaperman J, Landsberger S, Setoguchi Y (2003) Early Upper Limb Prosthesis Fitting: When and What Do We Fit. JPO2003 Vol. 15, Num. 1. pp. 11-17
Abstract: A survey of child amputee clinics in North America explored early fitting of children with unilateral below-elbow limb absence. Responses from 45 of 80 (56%) clinics revealed that most clinics prefer to fit at 6 months and add an active control system by 18 months. These are earlier ages than had been reported in the literature. Myoelectric hands with single site controls are often applied before 1 year. Responders indicated that child development guides the timing for initial fitting and the change to an active terminal device. Independent sitting is the most-used indicator for first fitting; awareness of cause and effect indicates readiness for activation. Passive hands are most often fitted initially. Approximately equal numbers of clinics prefer to use voluntary opening and voluntary closing terminal devices in the active fitting. Myoelectric hands are increasingly used. No significant differences were found between timing and terminal device preferences among clinics in various regions of the US and Canada and between Shriners and non-Shriners Hospitals. Financial considerations were not important in selecting the terminal device except in one-third of clinics at the time of activation. Parents are doing more of the training than was reported in the past, and few clinics use objective tests to measure outcomes of fitting. Responders identified many features they would like to include in a child's new terminal device. To read more: http://www.oandp.org/jpo/library/2003_01_011.asp
Back to top

PROFILE
Reinhold Reiter
The first myoelectric prosthesis we know of was created in the period 1944-1948 by Reinhold Reiter, then a physics student at Munich (Germany) University.
The system was controlled by a vacuum tube amplifier and was not portable. The hand was a modified Hüfner Hand that contained a control electro-magnet. The system was heavy, large, and not battery operated; the idea was to use it as a special prosthesis for use at a factory bench, powered from the nearest outlet. Reiter hoped that further development could make it portable.
Even at this early date Reiter recognized the need to obtain maximum information from the myoelectric signal: his system controlled both opening and closing of an electric hand from a single muscle.
Reiter's system did not gain clinical or commercial acceptance. Economic conditions in Germany after World War II prevented the work on myoelectric control from being continued there.
His work was not published, although it was described briefly in a report on a 1948 Hannover trade fair, printed in an obscure German medical newspaper. It was not discovered by the researchers who succeeded him until 1969, by which time his ideas had been reinvented.
Although Reiter conceived and developed the idea of myoelectric control in the early 1940's, others had the same idea later and apparently independently. The late Professor Norbert Weiner of Massachusetts Institute of Technology is reported to have suggested the concept around 1947. Berger & Huppert presented the idea in 1952. Battye, Nightingale, and Whillis at Guy's Hospital in London developed a myoelectric control system for a powered prosthesis in 1955 in what was for many years thought to be the first demonstration of this principle. That they were not first in no way detracts from their accomplishment. Soviet scientists were apparently the first to use transistors in a myoelectrically controlled prosthesis. The so-called Russian Hand was the first semi-practical myoelectrical limb to be used clinically and was sold (although not widely used) on a license basis for application in Great Britain and in Canada.
Sources:
"MEC 92," Proceedings of the 1992 MyoElectric Controls/Powered Prosthetics Symposium Fredericton, New Brunswick, Canada: August, 1992. Distributed under a Creative Commons Attribution-Noncommercial-No Derivative Works 3.0 United States License by UNB and the Institute of Biomedical Engineering, through a partnership with Duke University and the Open Prosthetics Project.
and
“Historical Aspects of Powered Limb Prostheses,” Dudley S. Childress, Ph.D.
LEGISLATIVE NEWS
Insurers Brace for Changing Policies
- Although ACA repeal is considered likely in the spring, a bipartisan coverage initiative could take its place.
Washington, D.C. – Health insurance companies’ short-term concerns around the unexpected victory of President-elect Donald Trump center largely on the government-run marketplaces he has pledged to eliminate.
The future of the Affordable Care Act (ACA) marketplaces is the leading concern of insurers, said Ceci Connelly, president and CEO at Alliance of Community Health Plans (ACHP).
“And specifically, not disrupting what is working,” Connelly said, referring to components of the marketplaces that have functioned well.
Although the marketplaces have been plagued by spiraling premiums heading into 2017 and by the departure of numerous insurers amid steep losses, the remaining participants have learned much about their enrollees over the last three years.
The incoming administration and Congress need to remember “the people who already have coverage, who are already getting medical care, who have doctors, who have prescriptions; we don’t want to upend that,” Connelly said in an interview. “We know from a business perspective that uncertainty is disruptive and very challenging as well.”
Uncertainty Reigns
Trump and the members of the incoming majority have repeatedly pledged to repeal the ACA marketplaces and much of the rest of the ACA, but have provided relatively little detail about how they will do that and what will replace the 2010 law.
Beyond the Trump campaign’s limited health policy report, many are looking to "A Better Way," the health policy framework issued in June by House Republicans led by Speaker Paul Ryan (R-Wis.).
“Ryan’s replacement model will, I suspect, be the first starting point in starting to discuss this,” former Speaker of the House Newt Gingrich said in a Nov. 10 conference call.
Such efforts by congressional Republicans to alter the ACA may be the best indicator of the likely next steps.
Another indication of how Congress may approach repeal is legislation that cleared Congress for the first time in December and was vetoed by President Barack Obama in January. The legislation used the tactic of reconciliation, which required only a majority vote in the Senate and therefore could not be stopped by Democrats. However the tactic limits repeal to tax- and spending-related provisions, such as the ACA marketplace subsidies and Medicaid expansion funding.
Vincent Ventimiglia, former assistant secretary for legislation at HHS, said the new Congress is likely to again pass such an ACA repeal measure within its first 100 days. So-called sidecar legislation, which would require Democratic support in the Senate, would accompany that repeal bill to provide the replacement plan.
Clay Alspach, a former chief counsel for the House Energy and Commerce Committee, said Medicaid expansion repeal is going to be especially contentious among House Republicans because many GOP governors, including Vice President-elect Mike Pence, approved the expansion in their states and don’t want to lose the coverage.
“Those members will be very resistant to repeal the Medicaid expansion unless there is some other way to cover those folks – there’s got to be a piece in place; there’s got to be a policy that’s put forward to give them a way to say, ‘We may be taking away your Medicaid expansion, but we will cover you this way or that way,” Alspach said in a conference call with industry clients.
Bipartisan Approach
That replacement plan is likely to involve a bipartisan approach “as much as possible,” Alspach said.
“We’re getting very strong indications they will try to make this bipartisan to some degree and that it will be a stepwise approach to reform, not a wholesale replacement,” Ventimiglia said on the conference call.
Importantly, the previously passed repeal legislation did not eliminate ACA marketplace funding or Medicaid expansion funding immediately and instead provided time before such cuts went into effect.
“There will be a transition period for those folks,” Alspach said.
A transition period would allow the federal bureaucracy time to prepare. For instance, Ventimiglia noted that any replacement system, such as a new system of tax credits to buy coverage, will require at least an 18-month lead-up time for the Internal Revenue Service to create a new regulatory framework.
Insurers and industry experts agreed that the transition period to any new coverage system would be critical.
“The Trump administration will have to run Obamacare for at least two years before they could possibly have a replacement in place,” said Robert Laszewski, a health insurance company advisor. “That means carriers—looking at an even more difficult 2018 open enrollment—will be very reluctant to participate. The Trump administration is going to have to subsidize carriers if they expect them to participate in 2018.”
Connelly agreed about the importance of a transition period. For example, the Trump administration will have to defend ACA cost-sharing reduction payments, which cover out-of-pocket costs for some enrollees and which the House of Representatives has successfully challenged in federal court.
Not Going Away
Among the healthcare policies enacted under Obama that Alspach expects to largely continue is the Medicare Access and CHIP Reauthorization Act of 2015 (MACRA), which was enacted with bipartisan support.
With MACRA, “You’re not going to see that level of change or disruption because you had both sides xx – Republicans and Democrats – coming together saying, ‘Let’s do this together’; they both want it to work, they both want their legacy to be a success,” Alspach said.
Interestingly, MACRA may have saved a key office in the Centers for Medicare & Medicaid Services (CMS), which House Republicans have previously targeted for elimination. That office, the Center for Medicare and Medicaid Innovation (CMMI), is seen by some as needed because it creates and oversees the advanced alternative payment models that physicians will be striving to join under MACRA.
However, a replacement law is likely to limit CMMI in several ways, such as by prohibiting it from using mandatory payment models and cutting its $10 billion appropriation for each future decade.
The repeal legislation that passed Congress also left out all of the ACA’s Medicare cuts, which are expected to continue under any Republican replacement. The cuts will be left in to pay for the new law and because the Medicare changes are seen as embedded in the healthcare system.
“I don’t think you’ll see a wholesale ‘Let’s go back to 2010’ because there’s just too much change that’s happened subsequent to 2010,” Alspach said.
Source:
http://www.hfma.org/Content.aspx?id=50762&utm_source=Real%20Magnet&utm_medium=Email&utm_campaign=105007631
Back to top

CONFERENCE
APTA Combined Sectional Meeting, Feb. 15-18, 2017, San Antonio
Association of Children’s Prosthetic-Orthotic Clinics (ACPOC) 2017 Annual Meeting March 22-25, 2017, Omni Houston Galleria Hotel, Houston.
Back to top

Q & A
Please feel free to submit your questions on Myoelectric Pediatric Prosthesis as well as any other issue you would like addressed.

Back to top

Educational Workshops and Inservices
Orthologix is available to present educational workshops and inservices for your group or your facility. Email us at info@orthologix.com to schedule.

We hope you have found this issue of the Orthologix E-news informative.
Thank you for your subscription.
Back to top
|